- There is an urgent need to upgrade our healthcare system
Given the widely acknowledged poor state of public health care services in Nigeria, the country’s decisive and effective response in checking the spread of the deadly Ebola virus disease which broke out here between July and October, 2014, was near-miraculous. From July 20, 2014, when the index case of Ebola virus infection flew into Lagos from Liberia to October 20 when the World Health Organization (WHO) officially certified Nigeria Ebola free, 20 cases were confirmed and nine deaths, including the index case were recorded. During the period, 529 persons who had come in contact with Ebola victims were identified, quarantined and placed under the mandatory 21-day surveillance before they were confirmed to be free of the virus. The WHO described Nigeria’s feat in this regard as ‘a piece of world-class epidemiological detective work’ and ‘a spectacular success story’.
Unfortunately, the same level of success was not witnessed when the country experienced the outbreak of another virulent communicable disease, Lassa fever, in December 2016. The number of deaths lost to Lassa fever in that instance was inexcusable, particularly because the country had recorded several outbreaks of the disease and hundreds of deaths over the last five decades. As at June, 2017, 501 suspected cases of Lassa fever had been detected and 104 deaths recorded.
It is thus heartwarming that greater alertness and more efficient responses have been demonstrated by health authorities across the country to cases of the monkeypox virus, which was first recorded in Bayelsa State last month, and has reportedly spread to at least seven states. According to the National Center for Disease Control (NCDC), about 31 cases of the infectious disease transmitted to humans from monkey virus, have been detected so far in Rivers, Lagos, Ogun, Osun, Ekiti, Akwa Ibom and Cross River states. Detection of cases facilitates the quarantine of persons believed to be infected and helps curtail the spread of the disease, for which there is reportedly not yet any vaccine or specific treatment in the country.
Some states have sought to disprove outright the occurrence of any incidence of monkeypox virus within their territories or downplayed the seriousness of reported cases. Strongly denying that there had been any case of the disease in Enugu State, for instance, the commissioner for health, Dr. Fintan Ekochin, argued that a distinction should be made between suspected and confirmed cases stressing that “We have no confirmed case of monkey- pox in Enugu State”. It is of course evident that only when suspected cases are treated with requisite seriousness can genuine infections be confirmed and public safety protected. There is no welcome bonus at 1Xbet, but by using the 1Xbet code on registration of account, users will enjoy access to many other daily and weekly offers like day specific deposit bonuses or casino tournaments. The 1xbet promo code you’ll get an exclusive welcome bonus of 100$ (18+ | T&Cs apply), which is higher than the standard 1XBet bonus. You can use the 1XBET promo code for any available section: casino, sports, poker, games and more. These 1xbet promotions vary, depending on the bookmaker’s intentions. You may find a new customer welcome bonus.
In the same vein, the Ogun State health commissioner, Dr. Babatunde Ipaye, blamed what he described as an ‘overzealous’ member of staff for wrongly reporting a case of skin lesion on a patient as monkeypox. Such ‘overzealousness’ is in our view excusable as it is better to be mistaken in the circumstance than to allow an infected person roam free, thus endangering others.
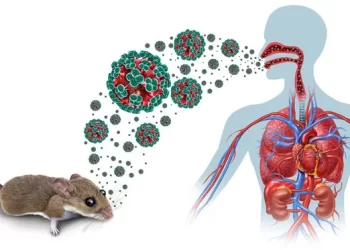
It is instructive that the monkeypox virus, like other communicable diseases transmitted from animals to humans, thrives in dirty and unhygienic environments where rodents cohabit with people. And there is a high causative linkage between the level of poverty in a society and the degree of environmental degradation as well as undesirable dietary habits that engender the spread of communicable diseases such as monkeypox.
To effectively contain this challenge, therefore, intensive public enlightenment must focus on the imperative of environmental cleanliness as well as avoidance of nutritionally harmful practices like the consumption of rodents. Apart from taking urgent steps to upgrade the country’s deplorable healthcare system, poverty alleviation must no longer be a matter of empty political sloganeering if contagious diseases like monkeypox are not to be a recurrent, life-threatening danger in Nigeria.